Genetic Testing for Inherited Cancer Risk
Introduction
Genetic testing has become an essential tool in modern oncology, enabling the identification of inherited genetic variations that increase an individual’s susceptibility to cancer. While most cancers arise from acquired mutations during a person’s lifetime, approximately 5–10% of cancers are linked to inherited genetic alterations.
Understanding these inherited risks allows for improved prevention, early detection, and personalized treatment strategies.
What Is Genetic Testing for Inherited Cancer Risk
Genetic testing for inherited cancer risk involves analyzing specific genes to identify pathogenic variants that may predispose an individual to cancer. These inherited changes are passed from parents to offspring and can significantly elevate lifetime cancer risk.
The presence of such mutations is often associated with hereditary cancer syndromes, which are characterized by: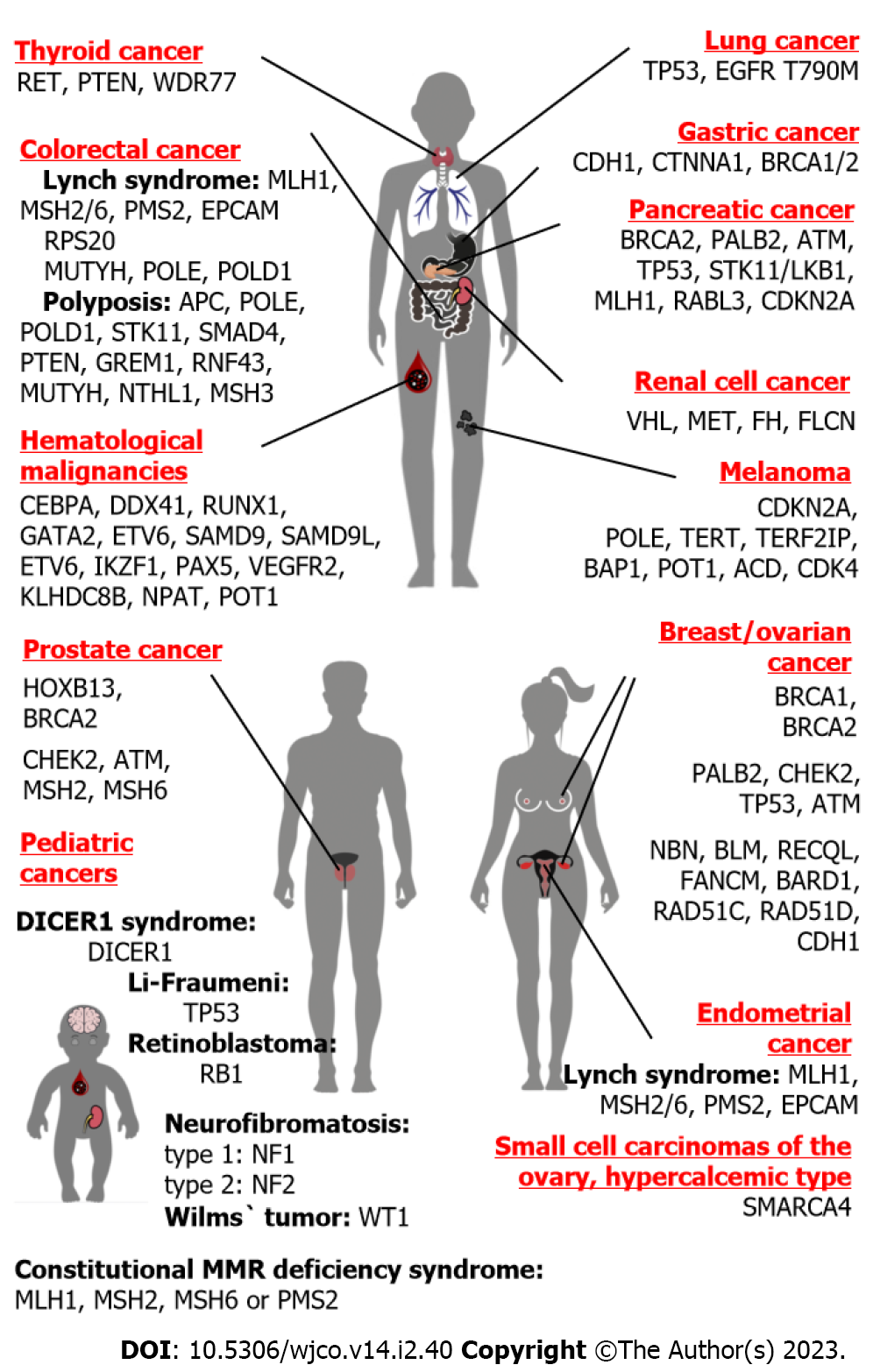
- Early onset of cancer
- Multiple cancers in the same individual
- Recurrence of similar cancers within families
It is important to distinguish inherited genetic testing from tumor genetic testing, which examines mutations acquired in cancer cells during a person’s lifetime and is mainly used to guide treatment decisions.
How Genetic Testing Is Performed
Genetic testing is typically recommended by a healthcare professional after evaluating an individual’s personal and family medical history.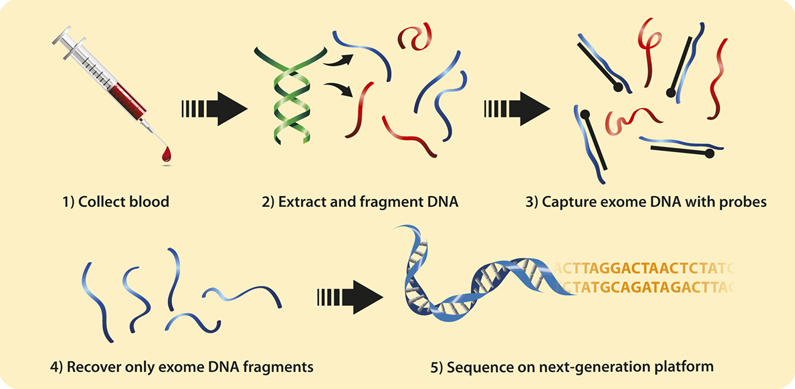
Sample Collection
Testing is conducted using biological samples such as:
- Blood
- Saliva
- Buccal (cheek) cells
- Skin cells
The sample is analyzed in a specialized laboratory, with results usually available within a few weeks.
Accessibility and Cost
In many cases, genetic counseling and testing are covered by health insurance when medically justified. For individuals without coverage, subsidized programs and support services may provide access to testing.
Who Should Consider Genetic Testing?
Genetic testing is recommended for individuals with certain clinical or familial indicators suggesting inherited cancer risk.
High-Risk Groups
Testing is strongly considered for individuals diagnosed with:
- Triple-negative breast cancer
- Ovarian cancer
- Pancreatic cancer
- Early-onset colorectal cancer
- Metastatic prostate cancer
- Male breast cancer
Family and Clinical Indicators
Additional factors suggesting hereditary cancer risk include:
- Cancer diagnosed at a young age
- Multiple cancers in one individual
- Repeated occurrence of cancer within a family
- Rare cancer types
- Known genetic mutations in relatives
In most cases, testing begins with a family member who has already been diagnosed with cancer to identify potential inherited mutations.
Types of Genetic Tests
Multigene Panel Testing
The most common approach involves multigene panels, which analyze multiple genes simultaneously. These tests are particularly useful when:
- No known mutation exists in the family
- Multiple cancer types are suspected
Targeted Testing
When a specific mutation is already identified in a family, testing may focus only on that variant or the entire gene associated with it.
Interpretation of Genetic Test Results
Genetic testing results can be categorized into several types:
Positive Result
Indicates the presence of a pathogenic genetic variant associated with increased cancer risk. This result can:
- Guide treatment decisions
- Inform preventive strategies
- Provide important information for family members
Negative Result
Indicates no detectable harmful mutation. However:
- A true negative confirms absence of a known family mutation
- An uninformative negative does not exclude risk if no known mutation has been identified
Variant of Uncertain Significance (VUS)
Represents a genetic change with unclear clinical relevance. Most VUS findings are later classified as benign, but ongoing monitoring is recommended.
Role of Genetic Counseling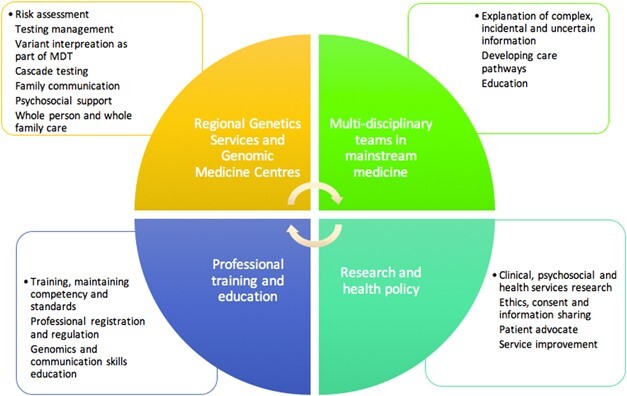
Genetic counseling is a critical component of the testing process. It is recommended both before and after testing to ensure proper understanding and decision-making.
Functions of Counseling
Benefits of Genetic Testing
Genetic testing offers several advantages:
- Identification of individuals at increased cancer risk
- Implementation of early screening and preventive strategies
- Personalization of treatment options
- Informed decision-making for family members
- Reassurance in cases of negative results
Limitations and Challenges
Despite its benefits, genetic testing presents certain limitations:
- Psychological stress and anxiety
- Uncertainty in interpreting some results ( VUS)
- Financial costs
- Need for long-term medical follow-up
- Potential privacy and discrimination concerns
At-Home Genetic Testing
The availability of direct-to-consumer (DTC) genetic tests has increased significantly. These tests allow individuals to collect samples at home and receive results without clinical supervision.
Limitations of At-Home Testing
- Incomplete analysis of cancer-related genes
- Limited clinical relevance
- Risk of misinterpretation
- Lack of professional guidance
Therefore, clinical genetic testing remains the most reliable option for assessing inherited cancer risk.
Ethical and Privacy Considerations
Genetic testing results contain sensitive information that may affect not only the individual but also their biological relatives.
Legal frameworks such as genetic non-discrimination laws aim to:
- Protect individuals from insurance or employment discrimination
- Ensure confidentiality of genetic data
However, individuals should carefully review privacy policies, especially when using commercial testing services.
Advances in Genetic Research
Ongoing research is continuously improving genetic testing through:
- Discovery of new cancer-associated genes
- Enhanced accuracy of variant classification
- Development of more sensitive diagnostic technologies
These advances aim to provide better risk assessment and more effective prevention strategies.
Conclusion
Genetic testing for inherited cancer risk is a powerful tool in preventive medicine and personalized healthcare. By identifying individuals with increased susceptibility to cancer, it enables targeted screening, early intervention, and improved clinical outcomes.
However, its effectiveness depends on proper interpretation, access to genetic counseling, and integration into comprehensive healthcare strategies. Continued advancements in research and technology will further enhance its role in cancer prevention and management.
Recent Posts
-
In Situ Hybridization in Cytogenetics
Introduction In situ hybridization (ISH) is a powerful technique used in cytogenetics to detect and …31st Mar 2026 -
The Evolution of the Anopheles Genome Project
Introduction Paludism remains one of the most serious infectious diseases worldwide, despite signifi …31st Mar 2026 -
Genetic Testing for Inherited Cancer Risk
Introduction Genetic testing has become an essential tool in modern oncology, enabling the identifi …31st Mar 2026


